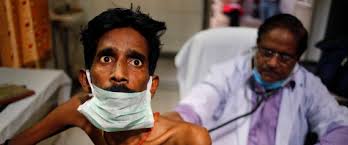
MUMBAI: After a slash in India’s healthcare budget and key public health initiatives, now the country’s ambitious tuberculosis control programme is facing a serious challenge, which could jeopardise supply of medicines, and lead to inadequate diagnostic services for TB patients.
The proposed funding cuts in the country’s TB control programme could lead to serious consequences like stock-outs of key TB medicines, and inadequate or shortage of specialised diagnostic kits, leaving patients in the lurch, and, in certain cases, to either face a relapse of the disease, or lead them to the dreaded drug-resistant form.
The fifth TB Joint Monitoring Mission 2015 in a draft report has observed that implementation of the National Strategic Plan (NSP) for the five-year period 2012-2017 is not on track, with vital procurements delayed and many planned activities not implemented
According to the Central TB Division, India has the highest burden of TB with two million cases every year, with over 60,000 drug-resistant TB patients.
Worse, the expansion of resources planned under the NSP which would triple the expenditure of the prior plan, has not been matched by allocation. While RNTCP expenditure has increased 27% since 2012, there is a growing gap between the allocation of funds and the minimum investment required to reach the goals of the Plan.
If this trend continues, final expenditure on the Plan would reduce to Rs 3,000 crore, or two thirds of the minimum of Rs 4,500 crore required, the draft report of the TB Joint Monitoring Mission 2015, a copy of which is available with TOI, warns.
It is not known whether the recommendations (of the draft) will be accepted by the government, experts say, adding that the JMM report may also be “modified”. The last JMM report came in 2012.
JMM members include international experts and donor partners (agencies like WHO, Gates Foundation, Global Fund) and national members (various stakeholders), officials from ministry of health, which reviewed India’s RNTCP from April 2015.
Says Dr Anant Bhan researcher, Global Health and Bioethics, “There is little doubt that there are major concerns about key national programmes like those of TB and AIDS control. With uncertainty about funding and budgetary cuts, there have been repeated stock-outs of drugs and diagnostics which could jeopardize the progress made in these programmes. Timely procurement and supply has also been a challenge for the programmes. It’s important to make them more efficient, and to ensure states also take more onus of healthcare funding, but abrupt changes without planning for the transition could push programmes such as AIDS and TB control into a crisis. It would of course also lead to the possibility of increased drug-resistance, a public health crisis India is already suffering from”.
Additional investment of at least Rs 750 crore annually will be required to reach the ambitious goals of the End TB Strategy. The government, along with WHO adopted the End TB Strategy in May 2014, which is crucial for the country as it bears a quarter of the global burden of the disease.
The scale-up of the TB control programme will be impacted, and many patients may go undiagnosed and continue to suffer with the infection, due to the shortage of specialised tests.
“Introduction of daily therapy in India’s DOTS programme has been long delayed by the Central TB Division, despite the guidance for immediate roll-out of daily therapy for HIV positive people by AIDS programme technical group two years back. With further budget cuts in TB programme, the adoption of daily TB regimen to curtail growing drug resistant TB among HIV positives still seems like a distant dream,” said Vikas Ahuja, President, Delhi Network of Positive People.
Not only that, the procurement and supply chain management continues to be a problem area with delays in procurement of GeneXpert (diagnostic), bad storage conditions and limited capacity of states. The report specifically mentions the 10 month stock outs of GeneXpert cartridges in Andhra Pradesh.
Worse, the JMM observed that two-thirds of the recommendations of JMM 2012 have not been fully implemented.